A sudden onset of floaters can be caused by a very serious eye problem and needs urgent attention, ideally within 24 hours. Read more about this here.
This page is for people who have bothersome longstanding vitreous floaters and have already been examined by an optometrist or eye surgeon in Melbourne to rule out a retinal tear or detachment.
What Are Floaters? How And When Do They Develop?
When we are born, the vitreous gel in our eyes is perfectly clear and fills the back of eye completely; light entering the eye passes through it undisturbed and is clearly focussed onto the retina. The vitreous is made up of about 99% water and 1% collagen. The tiny collagen fibres, or fibrils, are kept separate from each other by special molecules and this separation makes the vitreous remain both a gel and transparent.
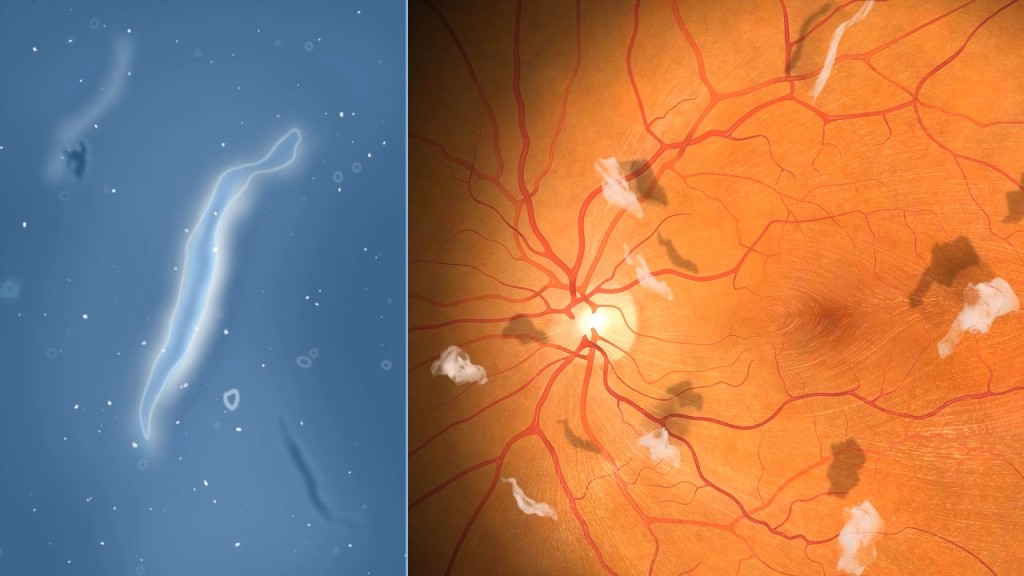
Over several years, the collagen fibrils clump together, with clear fluid filling the spaces between. This change is known as syneresis and occurs slowly from 20 to 70 years of age or older and happens earlier in short-sighted people. The clumps of collagen can block some light, cast shadows on the retina and be seen as floaters. Typically, these floaters look like dots, hairs, lines or clouds in the vision. They are most noticeable when looking at something bright or plain, such as a blue sky, blank computer screen or a white wall.
Floaters move around in the vitreous to a variable extent, lagging behind the eye’s movement and drifting around in the vision. It is because of the way in which they move, not their shape or appearance, that they are known as floaters. If they moved completely in time with eye movements and didn’t drift around, the brain would be able to ignore them and they would not be as bothersome.
Floaters’ effect on vision depends on their density, mobility and location in the vitreous itself.

What If Floaters Come Suddenly?
When people develop a posterior vitreous detachment (PVD), they often see new floaters or flashes of light, or both. It is very important that they are seen by their eye surgeon or optometrist in Melbourne within 24 hours to exclude retinal tear or retinal detachment. The floater that typically develops after a PVD is known as a Weiss ring. It is a dense ring that can look like a circle, oval or even break open to look C-shaped. It is made of collagen that was at the back of the vitreous, around the optic nerve, and moves forward when the vitreous separates from the retina.
Are Floaters Harmful?
No. The floaters themselves are not harmful.
How Long Do Floaters Usually Last?
After being examined, most patients are happy to find out that there is no serious sight-threatening problem, but many are quite upset to hear that it may take months for the floaters to go away. In fact, many floaters either drift out of view over time, being noticed only occasionally, or people simply become used to them, or both. This is obviously the ideal outcome and is, fortunately, what happens to most people.
For some people, however, the floaters persist, stay in the middle of their vision and affect their sight either constantly or intermittently. At the very least this is distracting, but it can stop people from reading, playing sport and driving. After many months or years of waiting for the floaters simply to go away or ‘get better’, many people in Melbourne choose to seek out treatment.
Can All Floaters Be Treated?
Large floaters that can be seen easily by both the patient and doctor are the easiest to treat. Sometimes, the floaters that bother a patient are not easily seen by the doctor. This is often because they are small and very close to the macula, where reflections make it difficult to see during an examination. In such circumstances, most doctors are reluctant to recommend treatments that have sight-threatening risks.
How Can Floaters Be Treated?
Put very simply, floaters can either be broken up or removed. The choice of which treatment is ideal and whether it’s worth trying one before the other depends on a number of factors. As with most medical or surgical treatments, it’s not just a case of which treatment works best, but a balance and trade-off between the potential risks and benefits of each. Doctors usually start from the ancient and always appropriate standpoint of “first do no harm”.
Your doctor should discuss the pros and cons of each of these options with you before you can make a decision about how you wish to proceed. Ideally, the doctor would be able to perform both forms of treatment; discussion of each individual’s risks of surgery is best done by a vitreoretinal surgeon in Melbourne who has examined the patient.
YAG Laser Vitreolysis
Nd-YAG lasers have been used in eye clinics since the early 1980s mainly to cut open a hole in a cloudy layer behind the lens implant used in cataract surgery. It works by focussing energy at a very small point in a short time and causing the tissue to turn into plasma, a state of matter that is different from solid, liquid or gas. When this happens, it is like an extremely small “lightning bolt” in the eye and a clicking sound can often be heard – many people feel as if someone is gently tapping the back or side of their head when being treated.
Before a treatment is performed, the pupils are dilated with drops that make it dangerous to drive home afterwards. More drops are put into the eye to anaesthetise the eye. Treatments can take up to 20 minutes at a time and involve the patient sitting at a laser, with their chin on a chinrest, forehead forwards against a strap and a contact lens being held on the eye by the doctor.
Sometimes a few different contact lenses are used in order to treat as many floaters as possible- it’s important for both the patient and doctor to be comfortable throughout.
Recent improvements in the laser optics, as well as the lenses used to focus the laser in the eye, mean that the laser can be applied to floaters in more parts of the vitreous, more safely and more precisely. The use of an extremely short pulse of laser (3 nanoseconds) is intended to vapourise, rather than just cut up, the floaters. As a result there are often tiny bubbles of gas released in the vitreous, which disappear within a few hours. Straight after a treatment, the vision will still be blurred and the floaters may look more broken up and less problematic.
It is very important to realise the following:
- Almost everyone needs 2 or 3 treatments.
- This is NOT A CURE for floaters. Even after successful treatment, there will still be some floaters, but hopefully nowhere near as bothersome.
- There are risks to this treatment, which are described below.
Throughout the procedure, frequent checks are carried out to be sure of where the laser is focussed, but complications can still occur. Whilst the laser is very precise, there is a definite risk of energy from the pulse moving towards the front of the eye and causing an immediate cataract. Whilst urgent cataract surgery can be performed, it may well mean that the best possible implant may not be used. If the laser energy extends to the macula and damages it, there may be permanent loss of central vision.
When treating floaters with laser in Melbourne, it’s sometimes impossible to tell whether the floaters are too close to the lens or macula to be treated safely until the contact lens is applied. Sometimes floaters can be moved away from the lens and macula simply by moving the eye and treating them in a ‘safe zone’. If not, the treatment has to be abandoned.
Vitrectomy Surgery
Vitrectomy can be performed if YAG laser vitreolysis either can’t be done safely or hasn’t been successful. Vitrectomy surgery is much more complex than laser vitreolysis and has significantly different risks. The procedure and its risks are described in detail here.
How Do I Decide Whether To Have A Treatment And Which To Have?
The decision over whether to have treatment or not is a very personal one and boils down to whether the risks of treatment weigh up against the potential benefit of treatment. The doctor’s role is to explain the risks and describe the potential benefits of each treatment in every patient’s case and guide the patient as to which is most likely to be beneficial. The patient then needs to decide whether the risks are worth taking; this is not a decision that most doctors will make for the patient and it can always be made after discussing matters with family or friends. Indeed, Dr Chauhan recommends that all patients bring someone into the consultation with them if at all possible. You will not be hurried into a decision.
Where Can The Treatments Be Done?
If you are seeing Dr Chauhan about your floaters, it is best if you are seen in his Boronia practice, located in the eastern suburbs of Melbourne. He performs YAG laser vitreolysis exclusively in the Boronia practice and vitrectomy surgery only at Box Hill.



